Pursuit's Take
After 2014 high profile controversy of wait times and access problems at VA medical centers, Congress appropriated $10 billion to the VA Choice fund, which allowed veterans to go outside the VA system to access health care. The program uses Third Party Administrators (TPA) to reimburse providers and the VA pays the TPA.
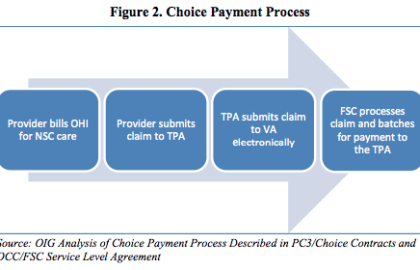
The Veterans Affairs Office of Inspector General issued a report on the timelines and accuracy of Veterans Choice program payments. The audit estimated that approximately 224,000 of the 2 million payments (12 percent) over a 2 period were improper and resulted in $39 million in overpayments. Additionally, the OIG estimated that the VA’s Office of Community Care (OCC) missed the 30-day prompt payment standard for half of the 2 million claims.
Some examples of improper payments include:
- Payment rate errors: “TriWest billed $977.00 for a Total Hip Arthroplasty procedure provided through the Choice Program. TriWest billed OCC using Current Procedural Terminology (CPT) code 27130 with an 81 modifier (Assistant at Surgery) for treatment provided on May 11, 2015. The contract medical claim processor determined that $223.02 was the correct Medicare rate for CPT code 27130 with an 81 modifier. OCC overpaid $753.98 for this service.”
- Other Health Insurance Payment (OHI) errors: “Health Net billed $160.34 for a claim for a therapeutic procedure provided through the Choice Program. We determined the treatment was not related to a service-connected condition or special authority and the veteran possessed billable OHI. OCC paid $160.34, the full Medicare rate, for the therapeutic procedure. In addition, Health Net reimbursed the provider $160.34 without any evidence of an offset for OHI.”
- Duplicate payments: “Health Net billed $40.76 for chiropractic care provided under the Choice Program. The December 17, 2014 chiropractic treatment was billed under CPT code 98940 (Chiropractic Manipulative Treatment) for $27.39 and CPT code G0283 (Electrical Stimulation) for $13.37. VA received a claim for this treatment on February 28, 2015 and it was paid on March 25, 2015. We compared this claim against paid non-VA care claims in our audit universe to determine if it was paid more than once. We identified a second claim in which OCC reimbursed the TPA $27.39 for CPT code 98940 with an AT (Active Treatment) modifier for the same veteran and provider performed on the same date. The second claim was also received by VA on February 28, 2015 and paid on March 25, 2015. We determined this payment to be a duplicate.”
- Pass-through errors: “Health Net billed and OCC paid $146.30 for inpatient hospital services provided through the Choice Program. Health Net billed OCC using CPT code 99232 (subsequent hospital care) for treatment provided on June 4 and 5, 2015. We reviewed the provider’s remittance advice and determined Health Net paid the provider $124.36 for this service but did not pass the discounted rate through to OCC. As a result, OCC overpaid the claim by $21.94.”
The OIG report concluded that “until OCC implements effective internal controls over Choice payments, OCC will continue to overpay TPAs for medical care. In addition, OCC needs to have effective performance standards in place to hold providers and TPAs accountable for complying with their contractual obligations.”
Take Homes
An audit of the VA Choice program estimated that approximately 224,000 of the 2 million payments (12 percent) over a 2 period were improper and resulted in $39 million in overpayments.